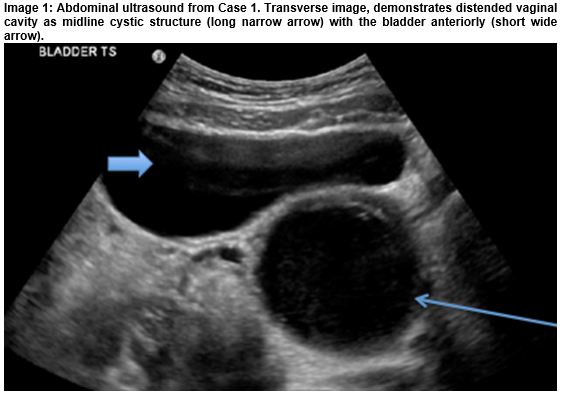
Atresia Hymenalis with Haematometrocolpos: A Benefit of Teaching a Case Series and Review of the Literature
L Whitla1, J Jones1, MJ Barrett1,2 , SM O’Donnell1,2, S Walsh1,2, C Blackburn1,2
1 Department of Emergency Medicine, Our Lady’s Children’s Hospital Crumlin.
2 Paediatric Emergency Research Unit, National Children’s Research Centre
Abstract
We present four cases of atresia hymenalis with resultant haematometrocolpos diagnosed in quick succession in the emergency department with a literature review.
Introduction:
Imperforate hymen or atresia hymenalis is a rare clinical presentation, the condition is estimated to be present in 0.5/1000 females1. It is the most common obstructive anomaly of the female genital tract, and results from failure of canalization of the vaginal plate in utero. Atresia hymenalis can present in neonates as bulging hymen due to accumulation of secretions by the uterovaginal mucosa2,3. Usually the imperforate hymen is asymptomatic until menarche, when haematometrocolpos results in symptoms such as abdominal pain, abdominal mass, urinary retention and constipation. Many cases are diagnosed in the evaluation of primary amenorrhoea or recurrent abdominal pain2,3. We present 4 cases diagnosed over a 7 month period in our ED.
Cases
Case 1: A 12-year-old girl with two months of severe lower abdominal pain radiating to hips and lower back with associated vomiting. Previous Emergency Department (ED) consultations for this pain resulted in the diagnosis of mesenteric adenitis and constipation. On her third attendance in 20 days, examination revealed Tanner stage IV breast development with a palpable, non-tender suprapubic mass. An abdominal ultrasound demonstrated a distended vaginal cavity (Image 1) and examination of the external genitalia showed an imperforate, bulging hymen. Urgent outpatient gynaecology review and surgical hymenotomy followed.
Case 2: An 11-year-old with three weeks of daily central, sharp intermittent abdominal pain which escalated, waking the patient from sleep and associated with dysuria and vomiting. A recent background history revealed multiple diagnoses of urinary tract infections from multiple health providers. Examination revealed Tanner Stage IV breast development, tender suprapubic mass, and bulging imperforate hymen of external genitalia. The diagnosis of atresia hymenalis with haematocolpos was made and confirmed by ultrasound. The patient was admitted for surgical hymenotomy.
Case 3: A 12-year-old with abdominal pain and a 24 hours of urinary retention after a transatlantic flight. Her history revealed 5 months of cyclical crampy abdominal pain for which she had attended health services in the United States. Examination revealed Tanner Stage IV breast development and supraumbilical palpable bladder. Urinary catheterisation drained 2.25L of urine and re-assessment revealed a suprapubic mass. The patient was admitted for investigation of abdominal mass. Abdominal ultrasound confirmed the diagnosis of haematometrocolpos. The patient had a surgical hymenotomy.
Case 4: A 12-year-old with two months of lower back pain, radiating to the hips with recent episodes of waking from sleep. The pain had a cyclical quality and an association with increasing constipation in the preceding fortnight. Urinary urgency and frequency were present. Positive examination findings included Tanner stage IV of breast development and non-tender mass in the supra-pubic region. A bulging, imperforate hymen was noted on examination of the external genitalia. A surgical review was requested and a diagnosis of imperforate hymen was subsequently confirmed by ultrasound. She underwent surgical hymenotomy.
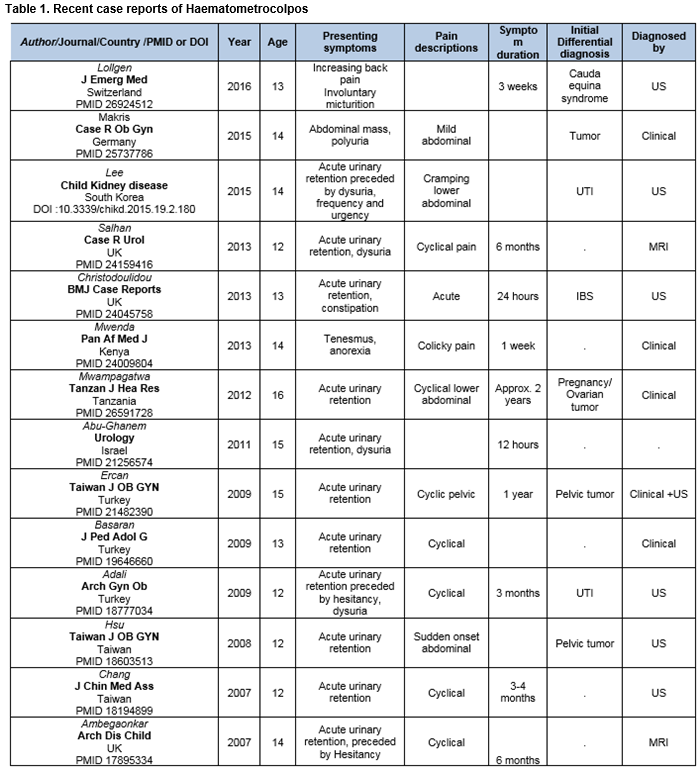
Discussion:
There is paucity of high quality publications on haematocolpos, with no prospective studies or large scale reviews to be found in the literature (Table 1). A review of existing literature (2007-2016) revealed the average age on presentation was 13.5 years, and cyclical pain preceding attendance was frequent (7/14, 50%) (Table 1). Acute urinary retention appears to be the commonest presentation in recent case reports2-9. In another case series urinary retention haematolcolpos was identified in three of the 28 cases (10.7%)10. Associated symptoms included urinary symptoms8, tenesmus5 and back pain3. Initial differential diagnoses were pelvic or abdominal tumours2, 4, 7, pregnancy6 and cauda equina syndrome3.
The diagnosis is often delayed, perhaps due to a failure to have a wide differential diagnostic list, to take a detailed gynaecological history or perform a thorough physical examination in a pubescent female9. Interestingly, the 4th case was identified clinically within hours following teaching on the three preceding cases in our ED. In summary atresia hymenalis with haematometrocolpos should be considered when evaluating premenarchal girls with secondary sexual characteristics presenting with lower abdominal pain, mass or urinary retention.
Correspondence:
Laura Whitla, Department of Emergency Medicine, Our Lady’s Children’s Hospital Crumlin.
Email: [email protected]
Conflict of interest:
The authors have no conflict of interest to declare
References:
1. Parazzini F, Cecchetti G. The frequency of imperforate hymen in northern Italy. Int J Epidemiol. 1990;19(3):763-4.
2. Makris GM, Macchiella D, Vaidakis D, Chrelias C, Battista MJ, Siristatidis C. Abdominal tumor in a 14-year-old adolescent: imperforate hymen, resulting in hematocolpos-a case report and review of the literature. Case Rep Obstet Gynecol. 2015;2015:429740.
3. Lollgen RM, Sabo J, Mettler A, Liniger B, Berger S. Unique Presentation of Hematometrocolpos Mimicking Cauda Equina Syndrome: Severe Back Pain and Urinary Incontinence in an Adolescent Girl. J Emerg Med. 2016.
4. Ercan CM, Karasahin KE, Alanbay I, Ulubay M, Baser I. Imperforate hymen causing hematocolpos and acute urinary retention in an adolescent girl. Taiwan J Obstet Gynecol. 2011;50(1):118-20.
5. Mwenda AS. Imperforate Hymen - a rare cause of acute abdominal pain and tenesmus: case report and review of the literature. Pan Afr Med J. 2013;15:28.
6. Mwampagatwa IH, Mponda BA. Imperforate hymen presenting with massive haematocolpos and acute urinary retention in a teenage girl: A case report. Tanzan J Health Res. 2012;14(4):293-6.
7. Hsu KP, Chen CP, Chien SC, Hsu CY. Hematocolpometra associated with an imperforate hymen and acute urinary retention mimicking a pelvic mass. Taiwan J Obstet Gynecol. 2008;47(2):222-3.
8. Adali E, Kurdoglu M, Yildizhan R, Kolusari A. An overlooked cause of acute urinary retention in an adolescent girl: a case report. Arch Gynecol Obstet. 2009;279(5):701-3.
9. Lee GH, Lee M-J, Choi YS, Shin JI. ImperforateHymen Causing Hematocolpos and Acute Urinary Retention in a 14-Year-Old Adolescent. Childhood Kidney Diseases. 2015;19(2):180-3.
10. Asgari SA, Mansour Ghanaie M, Simforoosh N, Kajbafzadeh A, Zare A. Acute urinary retention in children. Urol J. 2005;2(1):23-7.
(P623)