Potential Impact of Cycle of Care on Diabetes Services in Secondary Care
J Finnegan1, P McGing2, M Hatunic1
1Endocrinology Department, Mater Misericordiae University Hospital, Dublin
2Clinical Chemistry Department, Mater Misericordiae University Hospital, Dublin
Abstract
Diabetes Cycle of Care is a new initiative recently introduced by the Health Service Executive (HSE). In this review we found that a quarter of patients attending a secondary care diabetes outpatient clinic in a large teaching hospital could potentially be managed in primary care upon implementation of Diabetes Cycle of Care.
Introduction
Prevalence of Type 2 diabetes (T2DM) is increasing internationally and nationally1,2. Diabetes and its associated complications account for a significant workload and financial burden to the health service3. Optimising glycaemic control and managing cardiovascular risk factors reduces the risk of developing complications associated with diabetes4. The endocrine service in the Mater Misericordiae University Hospital provides specialist care to over 8000 patients with diabetes. As the prevalence of diabetes in Ireland is rising so is the demand for specialist care. The Diabetes Cycle of Care is a new initiative recently introduced by the HSE5. It will provide bi-annual structured diabetes review, through primary care services, for patients with type 2 diabetes with stable glycaemic control6. Our objective was to assess the proportion of patients attending diabetes clinics that have T2DM and analyse how many of them could potentially be suitable for the Cycle of Care.
Methods
We retrospectively audited ten consecutive outpatient diabetes clinics. Patients’ medical data was obtained using the hospital’s Electronic Patient Record (Patient Centre). Results of the most recent bloods tests for HbA1c, Lipids, and eGFR was gathered from the Laboratory Information System (Telepath v1.9). Information on the patients’ age, type of diabetes, and treatment, was obtained from clinic letters on Patient Centre. Data was analysed using Microsoft Excel to identify uncomplicated patients with T2DM, suitable for Cycle of Care, as per the ICGP guide including HbA1c <58 mmol/mol and eGFR >60 ml/min6.
Results
A total of 465 patients attended 10 diabetes clinics, approximately one-third (35.2%) of whom had Type 1 diabetes (T1DM) and two-thirds T2DM (64.3%) (Table).
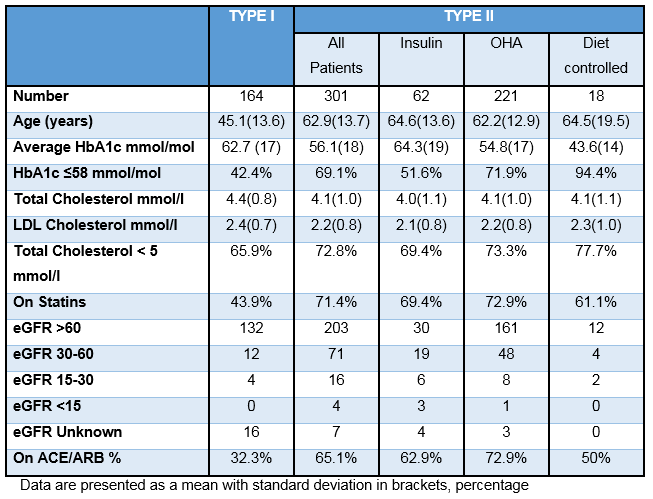
The average age of patients attending clinics with T1DM was 45.1 years. Mean HbA1c was 62.7(16.8SD) mmol/mol and 42.7% had an HbA1c of ≤58 mmol/mol. Patients with T1DM had average total cholesterol of 4.44 mmol/l; 67.1% had LDL less than 2.6 mmol/l. There were 43.9% patients with T1DM on lipid lowering therapy. The majority of patients with T1DM had an eGFR >60ml/min (80.5%), 7.3% had stage III CKD (eGFR 30-59ml/min) and 2.4% of patients had stage IV CKD (eGFR 15-29ml/min), just 32.3% were on an ACEi/ARB.
Patients with T2DM had an average age of 62.9 years with mean HbA1c 56.1 (17.7SD) mmol/mol. Just over a fifth (20.6%) of these patients were taking insulin, with 79.4% of patients using oral medication or diet to maintain glycaemic control. The average HbA1c in patients with T2DM on insulin was 64.3 mmol/mol compared to 53.9 mmol/mol in their counterparts taking oral hyperglycaemic agents (OHA)/ diet control. Hba1c of ≤58 mmol/mol was achieved by 51.6% of patients on insulin and 73.6% of patients taking OHA/diet alone. In patients with T2DM the mean total cholesterol was 4.10 mmol/l and 72.4% of patients had LDL cholesterol of less than 2.6 mmol/l. The majority of patients with T2DM are on a lipid lowering medication (71.4%). The prevalence of CKD was higher in patients with T2DM ; 30.2% have impaired renal function: 23.6% have stage III CKD (eGFR 30-59ml/min), 5.3% have stage IV CKD (eGFR 15-29ml/min), and 1.3% have stage V CKD (eGFR <15ml/min). There were 65.1% patients with T2DM treated with an ACEi/ARB. Interestingly 122 patients (26.2%) attending clinics with T2DM on OHA/diet, with intact renal function (eGFR ≥60ml/min) had a Hba1c of ≤ 58 mmol/mol .
Discussion
A high percentage (69.1%) of patients with T2DM achieved a target HbA1c of ≤ 58 mmol/mol and large numbers of patients were taking lipid lowering medication and ACEi/ARBs (65.1%). This review shows a significant number of patients with T2DM attending our specialist diabetes clinics are meeting their glycaemic targets. The majority of patients with T2DM are taking the appropriate medications to reduce cardiovascular risk.
Based on the data from this study 26.2% of patients currently attending the specialist diabetes outpatient clinics could be appropriately managed in primary care should the Cycle of Care be implemented. This positive development would allow specialist services to allocate more time and resources to managing patients with more complex disease.
Conflict of Interest:
The authors have reported no conflict of interest.
Correspondence:
Dr Mensud Hatunic, Consultant Endocrinologist
References
Endocrinology Department, Mater Misericordiae University Hospital, Dublin
Email: [email protected]
References:
1. Zimmet P, Alberti KG, Shaw J. Global and societal implications of the diabetes epidemic. Nature. 2001 Dec 13;414(6865):782-7.
2. Tracey ML, Gilmartin M, O'Neill K, Fitzgerald AP, McHugh SM, Buckley CM, Canavan RJ, Kearney PM. Epidemiology of diabetes and complications among adults in the Republic of Ireland 1998-2015: a systematic review and meta-analysis. BMC Public Health. 2016 Feb 9;16(1):132.
3. Danaei G, Finucane MM, Lu Y, Singh GM, Cowan MJ, Paciorek CJ, Lin JK, Farzadfar F, Khang YH, Stevens GA, Rao M, Ali MK, Riley LM, Robinson CA, Ezzati M. National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2 · 7 million participants. Lancet. 2011;378:31–40.
4. Stratton IM, Adler AI, Neil HA, Matthews DR, Manley SE, Cull CA, Hadden D, Turner RC, Holman RR. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ. 2000 Aug 12;321 (7258):405-12
5. New 'Diabetes Cycle of Care' service launched - IrishHealth www.irishhealth.com/article.html?id=24965
6. Irish College of General Practitioners (ICGP)– A Practical Guide to Integrated Type 2 Diabetes Care, 2016
(P552)
