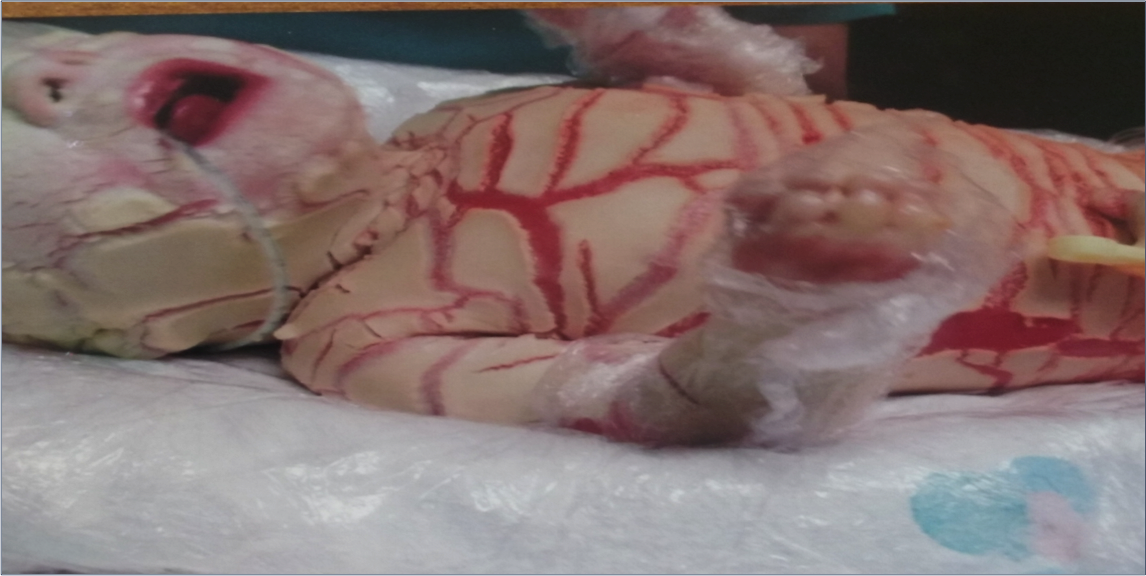
Harlequin Ichthyosis – A Case Report
Ugezu C H, Mazumdar A, Dunn E, Das A.
Department of Obstetrics and Gynaecology, Wexford General Hospital, Newtown Road. Wexford
Abstract
Harlequin Ichthyosis is a very rare genetic disorder affecting mainly the skin with severe morbidity and mortality. It affects both sexes with incidence of about 1 in 300,000 live births. Autosomal recessive inheritance has been inferred with mutation in ABCA 12 gene identified. Hence, genetic counseling and mutation screening of this gene should be considered in at-risk patients. Death usually occurred in the first 3 months of life due to sepsis, feeding problems and respiratory distress. With improved neonatal care and early introduction of retinoids, its survival rate has increased.
Introduction
Harlequin Ichthyosis is a very rare genetic skin disorder with severe morbidity and mortality. At birth the infant is born with a thick “coat of armour” that severely restricts movement. Autosomal recessive inheritance pattern has been inferred. Mutations in ABCA12 gene, a protein which plays a major role in the transport of lipids in the outermost layer of skin have been identified in a high percentage of Harlequin Ichthyosis children chromosomes1,3 . Historically the Harlequin Ichthyosis affected infant would die within two days of life because of feeding problems, bacterial infection and/or respiratory distress. However more recently a number of patients have survived because of developments in neonatal intensive care and the benefits of systemic retinoids. Successful management requires a multidisciplinary approach from the onset.
Case Report:
We report a case of 37-year-old para 2+0 who booked at 18 weeks gestation with EDD based on early scan of 14/11/15. She had two spontaneous normal vaginal delivery at full term and had no significant past medical or surgical history. Her serology results were negative. She had uneventful antenatal visits until at 34 weeks gestation when she presented with decreased fetal movement and pelvic girdle pain. On assessment CTG was reactive, umbilical artery doppler was normal and amniotic fluid index was 23cm. The baby was presenting as breech with an EFW on the 64th centile. She was reassured and discharged home with physiotherapy referral for her PGP. She was readmitted 10 days later at 35 weeks+ 6 days with PPROM, contracting three in 10 mins. On Vaginal examination cervix was 3 cm dilated. TAUSS confirmed oblique lie and hence decision made for category 2 Caesarean section following consultant review. At LSCS, female infant was delivered breech. The skin was very hard and thick with generalised deep fissures affecting the face, trunks, upper and lower limbs. Her birth weight was 3.14kg with APGAR 9 in one min and 10 in 5 mins. Placental swabs was taken and placenta sent for histology.
Baby was diagnosed with Harlequin Ichthyosis, and transferred to a tertiary centre for expert management. She unfortunately died after 11 days of supportive management. Placental swabs showed no growth and histology detected no abnormality.
Discussion
Reverend Oliver Hart became the first to document the condition Harlequin Ichthyosis in 1750. The disorder’s name alludes to the character Harlequin in the Italian Commedia dell’arte, which made its debut in the 1580’s2. Harlequin Ichthyosis is an inherited autosomal recessive disorder that is characterized by congenital epidermis abnormality. Mutations in the ABCA12 gene have been reported in the majority of Harlequin ichthyosis patients. The ABCA12 gene is believed to encode a transporter protein involved in the transport of epidermal lipids across cell membranes. Identification of this gene has made DNA-based prenatal diagnosis of Harlequin Ichthyosis possible. In order to express the disorder, individuals must inherit two recessive genes, one from each parent, although the parents (the "carriers") show no signs1,2,3. In the past, harlequin infants rarely survived the first few days of life. However, with recent advances in neonatal care especially with intense supportive care and administration of systemic retinoid therapy during the early neonatal periods, harlequin infants can survive. Just last year, 20-year-old Stephanie Turner who was born with the disorder gave birth to a perfectly healthy male infant.
The basic principles of management includes; meticulous skin care, hourly emollient, two hourly eye lubrication, monitoring for digital ischaemia secondary to constricted skin , nurse out of incubator in heated environment , fluid replacement, NG feeding. The crucial point is to start systemic retinoid eg Acitretin as soon as possible. Starting the retinoid before day three appears to improve survival as much as 80% (0.5-1mg/kg/day).(1,2,3)
Conflict of interest:
None declared
Correspondence:
Dr Chukwudi Ugezu, Department of Obstetrics and Gynaecology, Wexford General Hospital, Newtown Road. Wexford
Email: [email protected]
References;
1.Akiyama M, Sakai. K ,Sugiyama-Nakagiri Y, Yamanaka Y, McMillian JR, Sawamura D, Niizeki H, Miyagawa S, Shimizu H. Compound heterozygous mutations including a de novo missense mutation in ABCA12 led to a case of harlequin ichthyosis with moderate clinical severity. J Invest. Dermatol.2006 Jul;126(7):1518-23Epub 2006 May 4.
2. Hovnanian A. Harlequin ichthyosis unmasked: a defect of lipid transport. J Clin Invest.2005 Jul:115(7):1708-10. Review
3. Thomas AC, Cullup T , Norgett EE, Hill T, Barton S, Dale B A, Sprecher E, Sheridan E, Taylor AE, Wilroy RS, DeLozier C, Burrows N, Goodyear H, Fleckman P, Stephens KG, Mehta L, Watson RM, Graham R, Wolf R, Slavotinek A, Martin M, Bourn D, Mein CA, O’Toole EA, Kelsell DP. ABCA12 is the major harlequin ichthyosis gene. J Invest Dermatol.2006 Nov:126(11):2408-13 Epub 2006 Aug 10
P606