Hip Fracture and the Weekend Effect in an Irish Trauma Hospital
C. Downey, S. Flannery, A. Izydorczyk, J.F. Quinlan
Department of Trauma & Orthopaedics, Tallaght University Hospital, Dublin 24
Abstract
Aims
We examined the relationship between the 1-year mortality (OYM) rate and (i) those admitted at the weekend, (ii) those who underwent surgery at the weekend and (iii) those admitted during the NCHD changeover months (January & July) for the management of hip fracture in Tallaght University Hospital (TUH).
Methods
Admissions to TUH (2013 - 2016) with hip fracture (> 60 years old) were retrospectively examined. Data from the Irish Deaths and Events Registry was analysed to identify death events at 1 year. Logistic regression analysis was performed with respect to OYM with the three variables above.
Results
646 hip fracture patients were admitted (2013 – 2016). 178 (27.5%) were weekend admissions, 183 (28.4%) underwent weekend surgery and 93 patients (14.4%) were admitted during NCHD changeover months. There was no significant relationship between OYM and (i) weekend admission, (ii) weekend surgery or (iii) changeover admission in TUH.
Conclusion
This study offers the first examination of the weekend effect on fragility hip fractures and mortality in Irish patients and reports no significant weekend effect regarding 1-year mortality in this hip fracture cohort.
Introduction
Hip fractures represent one of the most common presentations to hospital of older patients (~3,600 per annum in Ireland1). Such patients form a uniquely vulnerable group within our healthcare system. Traditionally, orthopaedic trainees are taught that the OYM rate in this fragile population are ~30% at 1 year2. More recently, it was shown that this figure may be outdated and that 22% may be a more accurate, up-to-date estimation of OYM post fragility hip fracture3. Older patients with hip fractures present a significant challenge to Western healthcare systems. The oncoming “silver tsunami” of an increasing older population, both in terms of proportion and number, will see this issue only increase in scale and cost, both financial (estimated ~€14,400 per hip fracture4) and human. Eliciting the factors responsible for suboptimal outcomes in such patients is of critical importance to operate an efficient, excellent health service.
There are a number of national hip fracture registries5 which continuously collect and publish data in order to optimise delivery of care to those which suffer fragility hip fracture. In 2012, the Irish Hip Fracture Database was launched6 and publishes a national report annually which helps to measure, compare and improve the national hip fracture service delivery and outcomes. There have been 2 recent studies reporting improvements in 30-day mortality post hip fracture stemming from data collected by the National Hip Fracture Database in the United Kingdom. In 2015, a research group published data7 which suggested a significant improvement in 30-day mortality following the launch of a national clinician-led audit initiative. In 2017, the same group identified a significant and robust association between increased hours worked by orthogeriatricians and a reduction in 30-day mortality8.
Weekend admissions have previously been hypothesised to be an independent risk factor for increased patient mortality9. This phenomenon has been termed the “weekend effect” in the literature. It is of particular interest and debate in the UK as the National Health Service (NHS) introduces measures to implement their “seven day services” policy10. The intersection between the weekend effect and fragility hip fractures mortality has been examined in the internationally published literature. Since 2012, there have been 9 large studies examining the weekend effect and mortality in the fragility hip fracture cohort.
To our knowledge, the relationship between OYM and weekend admission/surgery and NCHD changeover admission has not been examined in Irish patients with respect to fragility hip fractures. We outline our findings in this paper.
Methods
The study cohort were collected retrospectively from all patient admissions to Tallaght University Hospital (TUH) between 2013 and 2016 due to new hip fractures in those over 60 years old. Admissions/surgical cases during the time period of 00:00 on a Saturday to 23:59 on Sunday were categorised as weekend admissions/surgical cases. All other admissions/surgical cases outside this time period were categorised as weekday. Admissions during the months of January & July were categorised as NCHD changeover admissions.
Access to the Irish Deaths and Events Registry was granted by the Department of Public Expenditure and Reform. Information from the registry was correlated with the local hospital information management software to establish death events at 1 year.
Univariate logistic regression analysis was performed on mortality at 1-year with three variables: (i) weekend admission, (ii) weekend surgery and (iii) admission during a NCHD changeover period. For analysis we used Stata SE (version 13, College Station Texas for PC) with a predetermined significance level of 0.05.
Results
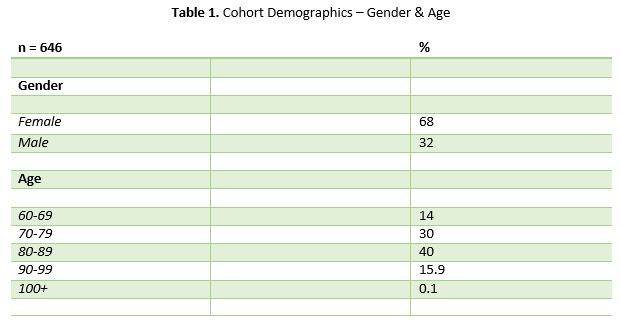
646 patients were admitted to Tallaght University Hospital with a single fragility hip fracture over a 4 year period (2013-2016) and are included in this study. 68% of the cohort were female (Table 1), 70% of patients were aged between 70-89 years of age (total range 60-101 years) and 76% of the cohort were admitted directly from their homes.
Of this total cohort of 646 patients, 178 patients (27.5%) were admitted at the weekend whilst 468 patients (72.5%) were admitted during the weekday period. 183 patients (28.4%) underwent surgery at the weekend whilst 463 patients (71.6%) underwent surgery during the weekday period. 93 patients (14.4%) were admitted during the NCHD changeover months January & July whilst 553 patients (85.6%) were admitted during the remaining months. The annual OYM (2013-16) for this cohort of hip fracture patients were as follows; 15.3%, 25.2%, 18.6% & 16.9% (mean 19%).
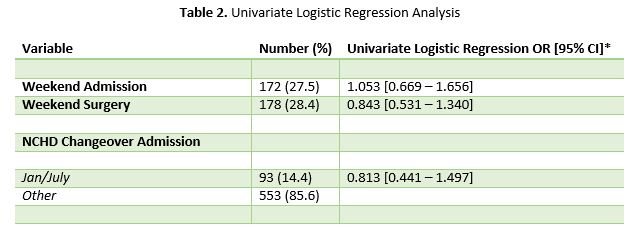
Univariate logistic regression analysis was conducted to examine the relationship, if any, between (i) weekend admission, (ii) weekend surgery & (iii) NCHD changeover month admission (Table 2). The odds ratio (OR) for weekend admission was 1.053 [0.669 – 1.656]. The OR for weekend surgery was 0.843 [0.531 – 1.340]. The OR for NCHD changeover month admission was 0.813 [ 0.441 – 1.497]. These results describe the impact of each variable on the observed event of interest, in this case OYM.
Strengths and Limitations
The strengths of our study include its access to the Irish Deaths Registry to follow patients to the one-year mortality endpoint. To our knowledge, we offer the first examination of the weekend effect on fragility hip fractures in an Irish population. Furthermore our findings are validated by other studies.
The limitations of our study include its sample size, study design and single centre. Retrospective studies such as this are also subject to bias and limited in the data available. Whilst our study incorporates the work of multiple surgeons, it relies on the activity of a single centre. There may be vast differences in the health status/ASA gradings of patients in different hospital catchment areas across Ireland. The average 80 year old patient in Dublin may not be comparable to the average 80 year old patient in Donegal. Provision of out-of-hospital care may vary widely and optimisation of such patients for surgery may be more or less complex when they reach hospital.
Discussion
Our study indicates there is no significant increase in OYM in our hip fracture cohort which were (i) admitted on the weekend versus those admitted on a weekday, (ii) underwent surgery on the weekend versus those who underwent surgery on a weekday and (iii) admitted during the NCHD changeover months versus those admitted over the remaining months. These findings are supported by the international literature with respect to this interesting topic.
A Canadian study11 published in 2001 is one of the most-cited early studies on the weekend effect. This group investigated the relationship between weekend admission and mortality in the top 100 leading causes of death. Whilst this group showed increased mortality for weekend admissions and a number of conditions (including ruptured abdominal aortic aneurysm, acute epiglottitis and pulmonary embolism), there was no significant difference in mortality regarding hip fracture patients (n ~ 60,000).
More recently, 2 research groups undertook separate retrospective studies12,13 investigating the weekend effect and mortality following hip fracture (n = 25,305 & 2989). Whilst these groups did not establish increased long term mortality rates (1-year), they both reported increased short term (30-day) mortality risk for all hip fracture patients (OR 1.4; p = 0.032 & OR 1.13; p < 0.05 respectively). On the same subject of 30-day mortality however, a British group14 recently investigated the effect of hip fracture and 30-day mortality and found no difference between those admitted on the weekdays vs. the weekends (n = 52,599).
There have also been 4 recent large studies which have investigated the weekend effect and hip fractures and have shown no association between either short or long term mortality (n = 1326, 1803, 816 & 38,020) 15-18.
Interestingly, a large American study19 (n = 344,989) reported statistically significant decreased short term mortality in those admitted at the weekend versus the weekday (OR 0.94, 95% CI 0.89 – 0.99). Such a study offers an unusual new paradigm for the weekend effect and piques interest in what may be the hidden benefits of the same.
More studies which specifically investigate hip fracture mortality and weekend surgery/admission during NCHD changeover months would be welcomed. The OYMs in TUH are inline with international standards.
In conclusion, the weekend effect should be taken to represent a complex constellation of factors, including limited availability of experienced staff, surgeon fatigue and reduced availability of resources in hospital. Eliciting and eliminating the negative factors behind our weekend services is required to optimise outcome, rather than simplistic comparison of opening hours and availability akin to commercial retail and business services. Nonetheless, to our knowledge this study offers the first examination of the weekend effect on fragility hip fractures of Irish patients. We demonstrate that in our institution, there is no evidence of any weekend effect on OYM.
Conflicts of Interest Statement
The authors have no conflict of interest to declare.
Corresponding Author
Dr. Colum Downey
Department of Trauma & Orthopaedics,
Tallaght University Hospital,
Dublin 24
Ph: (01) 414 2000
Email: [email protected]
References
1. Irish Hip Fracture Database National Report 2016 [Internet]. 2019 [cited May 2019]. Available from: https://www.noca.ie/wp-content/uploads/2015/04/Irish-Hip-Fracture-Database-National-Report-2016-FINAL.pdf.
2. Moran, C.G., Wenn, R.T., Sikand, M., Taylor, A.M. Early mortality after hip fracture: is delay before surgery important? J Bone Joint Surg Am. 2005; 87(3):483-9.
3. Downey, C., Kelly, M., Quinlan, J.F. Changing trends in the mortality rate at 1-year post hip fracture – a systematic review. World Journal of Orthopaedics. 2019; 10(3):166-175.
4. Gannon, B., O’Shea, E. and Hudson, E. (2007). The economic cost of falls and fractures in people aged 65 and over in Ireland. Technical Report. Irish Centre for Social Gerontology, National University of Ireland, Galway.
5. Johansen, A., Golding, D., Brent, L., Close, J., Gjertsen, J.E., Holt, G., et al. Using national hip fracture registries and audit databases to develop an international perspective. Injury. 2017; 48(10):2174-9.
6. Audit NOCA. Irish Hip Fracture Database National Report 2016.
7. Neuburger, J., Currie, C., Wakeman, R., Tsang, C., Plant, F., De Stavola, B., et al. The impact of a national clinician-led audit initiative on care and mortality after hip fracture in England: an external evaluation using time trends in non-audit data. Med Care. 2015; 53(8):686-91.
8. Neuburger, J., Currie, C., Wakeman, R., Johansen, A., Tsang, C., Plant, F., et al. Increased orthogeriatrician involvement in hip fracture care and its impact on mortality in England. Age Ageing. 2017; 46(2):187-92.
9. Rimmer, A. Weekend Effect is not reduced by clinical standards designed to tackle it. BMJ. 2017 (j5185):359.
10. Seven Day Services in the NHS: National Health Service; 2017 [Available from: https://improvement.nhs.uk/resources/seven-day-services/.
11. Bell, C.M. & Redelmeier, D.A. (2001). Mortality among patients admitted to hospitals on weekends as compared with weekdays. N. Engl. J. Med. Aug; 345 (9):663-8.
12. Thomas, C.J., Smith, R.P., Uzoigwe, C.E., Braybrooke, J.R. The weekend effect: short-term mortality following admission with a hip fracture. Bone Joint J. 2014; 96-B(3):373-8.
13. Kristiansen, N.S., Kristensen, P.K., Norgard, B.M., Mainz, J., Johnsen, S.P. Off-hours admission and quality of hip fracture care: a nationwide cohort study of performance measures and 30-day mortality. Int J Qual Health Care. 2016; 28(3):324-31.
14. Neuburger, J., Currie, C., Wakeman, R., Georghiou, T., Boulton, C., Johansen, A., et al. Safe working in a 7-day service. Experience of hip fracture care as documented by the UK National Hip Fracture Database. Age Ageing. 2018; 47(5):741-745.
15. Sheikh, H.Q., Aqil, A., Hossain, F.S., Kapoor, H. There is no weekend effect in hip fracture surgery - A comprehensive analysis of outcomes. Surgeon. 2017; 16(5);259-264.
16. Nijland, L.M.G., Karres, J., Simons, A.E., Ultee, J.M., Kerkhoffs, G., Vrouenraets, B.C. The weekend effect for hip fracture surgery. Injury. 2017; 48(7):1536-41.
17. Mathews, J.A., Vindlacheruvu, M., Khanduja, V. Is there a weekend effect in hip fracture patients presenting to a United Kingdom teaching hospital? World J Orthop. 2016; 7(10):678-86.
18. Daugaard, C.L., Jorgensen, H.L., Riis, T., Lauritzen, J.B., Duus, B.R., Van der Mark, S. Is mortality after hip fracture associated with surgical delay or admission during weekends and public holidays? A retrospective study of 38,020 patients. Acta Orthop. 2012; 83(6):609-13.
19. Boylan, M.R., Rosenbaum, J., Adler, A., Naziri, Q., Paulino, C.B. Hip Fracture and the Weekend Effect: Does Weekend Admission Affect Patient Outcomes? Am J Orthop (Belle Mead NJ). 2015; 44(10):458-64.
Issue: Ir Med J; Vol 112; No. 6; P949
